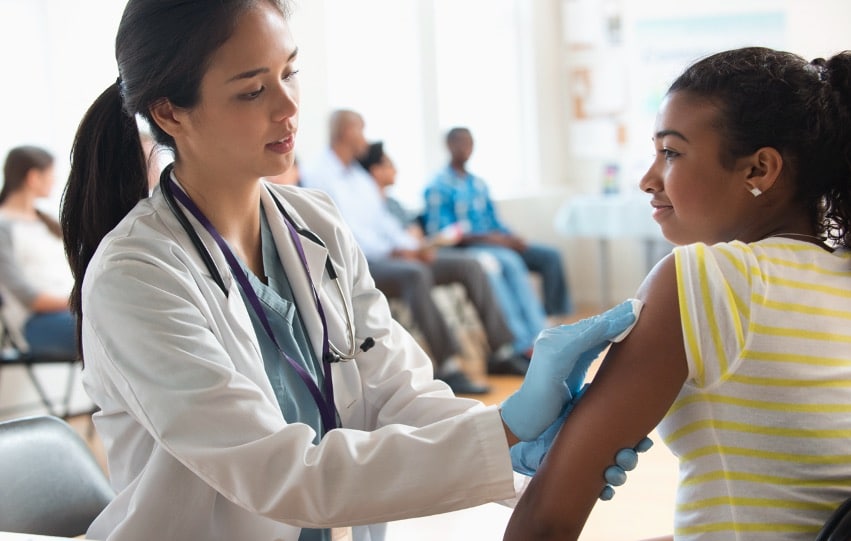
In a nationwide survey of almost 1,000 young people ages 14 to 24, MyVoice findings suggest young people most value a doctor’s personality and empathy over racial/gender concordance or sociodemographics — although they do serve as an important factor in some clinical encounters.
As one respondent put it, “No, I don’t care about my physician’s physical/social traits aside from personality. They need to be kind and considerate, but aside from that, I don’t care if they’re male, female, old, young, disabled, normally abled, poor, rich, white, black, brown or even green! As long as they are a good person who cares, understands, and offers scientific treatment, I am happy with them.”
A team of MyVoice researchers recently published their complete findings in BMC Primary Care with the paper, “Youth preferences for healthcare providers and healthcare interactions: a qualitative study.”
MyVoice is a nationwide, ongoing, open-ended text messaging survey of youth, which gathers perspectives from 14- to 24-year-olds on a variety of health and policy issues.
While previous literature has suggested that trust, knowledge, regard, and loyalty play a part in effective clinical encounters – as well as patient-physician social concordance – less is known about the role of patient-provider concordance on health outcomes among adolescents and young adults.
“The aim of this study was to understand youth perspectives of their relationships with their healthcare providers and the importance of sociodemographic similarities and differences as reported by youth,” wrote the MyVoice authors, which included first author Marika Waselewski, MPH, who also serves as MyVoice program manager. Co-authors included team members Xochitl Amaro, Ryan Huerto, Jessica Berger, Marcus Spinelli da Silva, Kate Siroky, Anthony Torres and MyVoice Director Tammy Chang, MD, MPH, MS, associate professor in the Department of Family Medicine at the University of Michigan.
Via text message, researchers contacted 1,163 youth members of the MyVoice cohort. A total of 944 participants responded to at least one question. Questions included:
- What do you look for when choosing a doctor?
- Is it important that you have similar characteristics to your doctor (age, gender, race/ethnicity, disability, background, personality, etc.)?
- When would being similar to your doctor be important? Specifically, for what type of healthcare visits?
- How would being similar to your doctor impact what you say or do during your visit?
- If you were in a situation where you felt uncomfortable with your doctor, what could they do to make you feel more comfortable?
Based on qualitative results, three themes emerged:
- Youth most value personality, professionalism, accessibility, and a healthcare provider’s clinical training.
- Youth most commonly said concordance was important in regard to gender, particularly among female individuals and for sexual health-concerns. Racial concordance was differentially important to respondents as well, with non-white individuals more likely to prefer racial concordance. However, almost half of respondents said personality and relationship quality were more important to them.
- Respect and open communication make youth feel more comfortable. However, some youth said they would simply switch providers if they didn’t feel comfortable.
“Greater understanding of youth perspectives on patient-physician relationships can inform programs and policies that improve youth engagement in healthcare and health outcomes,” Wasalewski et al write. “Programs that assess and strengthen professional and interpersonal skills such as listening and cultural humility may improve engagement and satisfaction among adolescent and young adult patients, particularly non-white and female patients.”
Article cited: Waselewski, M., Amaro, X., Huerto, R., Berger, J., Spinelli da Silva, M., Siroky, K., Torres, A., & Chang, T. (2024). Youth preferences for healthcare providers and Healthcare Interactions: A qualitative study. BMC Primary Care, 25(1). https://doi.org/10.1186/s12875-024-02300-z
